Age-Related Macular Degeneration (AMD)
AMD Specialist
Age-related Macular Degeneration (AMD) is a disease, which causes visual loss in patients over the age of 50. The vision loss is painless, usually gradual and not severe, but can be variable among patients. Macular degeneration is named for the macula, the part of the retina responsible for central vision. Peripheral vision is usually not affected by macular degeneration and often, this illness will go unnoticed until a patient engages in a task such as driving or reading, in which central vision is crucial. As the term “degeneration” implies, the illness becomes more noticeable over time and tends to get worse with or without treatment. Macular degeneration typically affects adults over 65 and the main risk factors for the disease are increasing age and genetics (family history of macular degeneration). Smoking, high cholesterol and hypertension are also risk factors. This disease does not cause total blindness and most macular degeneration patients can see well enough to care for themselves.
Symptoms Of Macular Degeneration:
- Blurred, dim, wavy or distorted vision
- A black spot in front of central vision
- Difficulty reading or driving
Because macular degeneration usually occurs in one eye before the other, a patient may only notice the symptoms upon covering one of their eyes. To test for Macular degeneration, your eye care provider may use an Amsler grid macular degeneration test (a test that can also be done at home by the patient to monitor symptoms).
Types of Macular Degeneration:
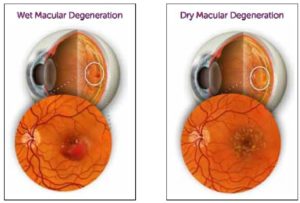
Little is known about the causes of macular degeneration, except that it pertains to aging in specific retinal layers. Macular degeneration occurs in two forms: exudative (“wet”) and atrophic (“dry”). Most cases, 90% in fact, are dry– the less severe form. However, dry macular degeneration occasionally evolves into the more severe wet macular degeneration. Wet macular degeneration causes a faster and more severe form of visual loss.
Treatment from an AMD Specialist
As the population’s life expectancy grows, macular degeneration is becoming a greater health concern and more medical researchers are devoting more energy to treating this illness. Unfortunately, macular degeneration has few treatment options. However, the Age-Related Eye Disease Study (AREDS 2) shows that anti-oxidants and caratenoids such as Vitamins C, Vitamin E, Zeaxanthin, Lutein and minerals such as copper and zinc, help slow the disease’s progression when it reaches the intermediate phase (AREDS 2 eye vitamin).
For wet Macular degeneration, laser photocoagulation or photodynamic therapy (PDT) may be an option. In this particular treatment, an intense light is used to focus on and close areas of leakage that are linked to wet macular degeneration. Most patients are not a candidate for laser or PDT unless the leakage is outside the center of the macula or the leakage is unresponsive to the standard medicine injections (discussed momentarily). In cases where the leakage is within the center of vision, patients may consider another treatment. One approach may be the new class of drugs known as anti-VEGF (anti vascular endothelial growth factor) that are injected into the vitreous cavity. These drugs include:
- Ranibizumab (Lucentis®)
- Alfibercept (Eylea®)
- Bevacizumab (Avastin®)
Injecting these medicines into the center of the eye helps reduce the prominence of actively growing blood vessels in the outer retina. This in turn can reduce the risk of further vision loss and in some patients, actually improve their vision. All forms of wet macular degeneration treatment are most effective when applied early on in the disease process. The leakage is easiest to target when localized, as in the early stages of macular degeneration. Therefore early diagnosis is key to managing and preventing the progression of this disease.
Contact Our AMD Specialist Today!
If you feel you have taken the Amsler grid test and are concerned about your results, or have other reasons to suspect you are suffering from macular degeneration contact Retina Associates of Orange County today. Retina Associates of Orange County‘s qualified retinal specialists can help restore your sight.
As a specialist who has experience treating age related macular degeneration AMD can discuss with you, the symptoms of serious eye issues and disorders can be hard to identify. Age related macular degeneration, or AMD, is a common disease in many aging or elderly adults, and typically occurs after age. Identifying the early signs and symptoms of AMD is essential so that it can be managed before it progresses to a more severe stage. The more it progresses, the more difficult it will be to treat. It is a condition that is less well-known, but a retina specialist can explain to you more about it and what to expect if you are diagnosed.
What is Age Related Macular Degeneration (AMD)?
AMD stands for age related macular degeneration. The name, macular degeneraiton denotes a condition that comes from the macula in the eye, located in the retina, where part of it begins to deteriorate. There are several forms of AMD: wet AMD or dry AMD . One or both eyes can be affected, but it usually develops in one eye first. Since the middle area of the eye is where degeneration occurs, loss of vision is in the center of the eye. Peripheral vision is largely unaffected by age related macular degeneration. However, it can make tasks and activities like reading, gardening, driving, and other everyday tasks difficult to do. Patients with AMD may not even be able to drive at all if their condition is especially severe. There are several factors that can contribute to the development of AMD, such as age, genetics and unhealthy lifestyle choices.
Is Macular Degeneration Treatable?
As a qualified age related macular degeneration AMD specialist can go over in detail, AMD is treatable if action is done as soon as possible. There is both wet and dry AMD, and currently there are only treatments available for wet AMD. Dry AMD can be treated and progression of the disease can be slowed down. Talk to a retina specialist to obtain more information about possible treatments for you.
Signs of Macular Degeneration
Being aware of the common signs of AMD is necessary so that you can seek treatment before the disease progresses. Patients who are diagnosed with age related macular degeneration may experience one or more symptoms, such as the following:
- Wave or straight lines
- Dark spots in their vision
- Blurry or distorted vision
Macular degeneration is a serious eye condition that should not be ignored. If you suspect even minor symptoms, you should call an eye doctor who is familiar with macular degeneration and treatments for it. Describe any symptoms that you see to an eye doctor and they will conduct additional tests if necessary. They will do a complete exam to see what symptoms you have and treatments for your condition.
See an Eye Specialist
AMD is a disease that can drastically impede your day to day life and impact the health of your eyes. Seek treatment immediately so that an eye doctor can run tests and identify potential treatments for you. Talk to a qualified and experienced age related macular degeneration AMD specialist now.
Newport Beach Macular Degeneration Doctor | 5 Facts About Macular Degeneration
