Laguna Hills Retinal Vein Occlusion (RVO) and Macular Edema
Retinal Vein Occlusion
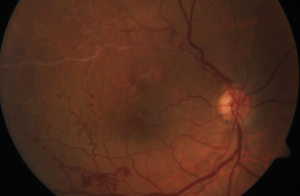
The retina is the light-sensing layer of cells that lines the inner wall of the back of the eye. The retina converts light into signals that are sent to the brain where they are recognized as images.
What is Retinal Vein Occlusion?
Your retinas require a rich supply of oxygenated blood. This blood is carried to the retina from the heart through arteries, while veins carry deoxygenated blood from the retina back to the heart via the optic nerves. The arteries that transport oxygen to your retina may stiffen and thicken over the years, especially in people with diabetes, cardiovascular disease, high blood pressure and high cholesterol. The retinal arteries and veins are close to the optic nerve and cross various locations on the retina’s surface. As arteries thicken, they can compress the retinal vein at artery-vein crossing points or in the optic nerve. This compression can be so severe that the veins become constricted and thus blood flow to the heart is reduced. The blood then backs up into the retina not unlike the water in a clogged bathtub. The pressure of blood in the veins causes swelling (called macular edema) and bleeding in the retina. There are three kinds of retinal vein occlusions:
- The most commonly seen cases are branch retinal vein occlusions, in which the blockage occurs in a smaller vein on the retina’s surface. The consequent hemorrhaging and swelling may result in diminished vision if the macula, the retina’s center, is involved.
- The second most common form of retinal vein occlusion is a central retinal vein occlusion in which the main retinal vein is blocked within the optic nerve. This is usually a more severe kind of occlusion that causes hemorrhages and swelling throughout the retina. This often leads to a more serious decrease in sight.
- Less common is hemi-retinal vein occlusion, in which the vein draining one-half of the venous circulation is occluded. Generally, this is more severe than the branch retinal vein occlusion but less so than central retinal vein occlusion
Eyes with retinal venous occlusive disease may develop macular edema (retinal swelling), or growths of fragile, abnormal blood vessels on the retina’s surface. These growths can cause bleeding into the vitreous gel. This bleeding is typically associated with the sudden appearance of floaters or severe loss of vision. Patients with central retinal vein occlusions may also develop abnormal blood vessels on the iris. These blood vessels can cause a severe form of glaucoma known as neovascular glaucoma.
Fortunately, retinal vein occlusion is usually only present in one eye so the other eye remains unaffected.
What are the risk factors for retinal vein occlusions?
The main risk factors include: high blood pressure, diabetes, high cholesterol, cardiovascular disease, glaucoma, and other blood disorders. Some patients have no risk factors and a more extensive work-up to determine underlying cause may be warranted.
Symptoms of Retinal Vein Occlusion
People with a retinal vein occlusion may not exhibit symptoms but those who do may have a sudden onset of blurred vision in one eye. However, blurred vision is a symptom of many ocular conditions. Therefore, one will have to undergo testing to confirm that one has retinal vein occlusion.
Treatment for Retinal Vein Occlusion
There are numerous treatment options to reduce the risk of vision loss in cases of retinal vein occlusion. For those with macular edema resulting from this condition, laser photocoagulation may help. Anti-vasccular endothelial growth factors (anti-VEGF) drugs such as ranibizumab (Lucentis), bevacizumab (Avastin) or aflibercept (Eylea) may be injected into the vitreous gel to treat the swelling associated with this condition.
Like many medical conditions, the treatment is done to manage the disease and reduce the risk of worsening. Thus, with intravitreal injections, patients may require life-long treatment.
Retina specialists can treat patients with the more severe kind of venous occlusive disease (neovascular glaucoma) with scatter laser to the retina and/or continued injections in hopes of stabilizing the disease process and preventing severe vision loss or blindness.
As retinal vein occlusions are typically associated with high cholesterol, diabetes and high blood pressure, monitoring and treating these medical conditions are important in those patients with venous occlusive disease. Thus, following up with your primary care doctor is imperative.
Contact Our Eye Doctors for Help with Retinal Vein Occlusion or Macular Edema
To learn more about venous occlusive disease and how our retina specialists can help, contact our physicians at Retina Associates of Orange County.
How Vision is Impacted
Retinal vein occlusion and related diseases can result in serious long-term damage not just to your retina, but the rest of your eyes. Because the retina is affected by blood clots, you may have difficulty processing light or adjusting your eyes to light. Loss of vision can occur gradually or quickly depending on the severity of the condition. When the retina has this kind of damage, signals to the brain are not able to be processed correctly, leading to trouble identifying images since they cannot be focused properly.
A macular edema is just one way that vision is affected by retinal vein occlusion. The macula is located inside the retina and is responsible for keeping vision focused. When this part of the retina is swollen because of the overflowing blood, blurry vision can occur. In extreme cases, blindness can result as well.
Reducing Your Risk
There are some effective things that a patient who is at high risk of developing retinal vein occlusion can do to avoid developing the condition. Doing frequent exercise several times a week and eating a balanced and nutritious diet can greatly reduce the chances of getting the disease. If you have a family history of high blood pressure, blood disorders, cardiovascular issues, or other health issues, taking active steps to improve your health can make a huge difference. For more information about preventative measures you can implement in your life, you can turn to an eye doctor for guidance.
Ways To Treat Retinal Vein Occlusion
In order to treat retinal vein occlusion, an eye doctor may consider several options. A commonly used treatment that has proven to be effective are prescription drugs to help combat the swelling from the blood flow. However, it is not a one-time treatment or even multiple sessions. The patient may have to continue undergoing the treatment for the rest of their life to manage their symptoms, as a trusted doctor who does treatments for Laguna Hills retinal vein occlusion RVO and macular edema can explain. Talk to a trusted doctor to find out available treatment options that could be right for you.
Meet With an Eye Doctor
Any kind of eye complications can be hard to live with, but if you have a serious condition like retinal vein occlusion, it is possible to mitigate the effects and consequences if you seek treatment right away. You should take this condition seriously and talk to an experienced doctor so you can begin exploring your options. Your condition may be in the early stage, so there could be multiple ways that your symptoms can be alleviated. Do not think that it is too late to save your vision if you think that you have a retinal vein occlusion and other retinal issues.
When you go to an experienced eye doctor who can help you discover suitable treatments, you can preserve the health of your eyes and reduce vision loss. Find out more about Laguna Hills retinal vein occlusion RVO and macular edema services in your area now so you can schedule a consultation.
